Two new suspected cases of hantavirus were reported Friday — one in Spain and another on Tristan da Cunha — widening the geographic footprint of an outbreak that began aboard a luxury cruise ship in the South Atlantic. The locations are thousands of miles apart, underscoring how far passengers had traveled after disembarking.
Health officials say the expanding list of suspected infections brings renewed attention to a cluster already linked to three deaths, though the World Health Organization maintains that the overall risk to the public remains low. The virus, believed to be the Andes strain, does not spread easily between people, and most transmission is still thought to occur through contact with infected rodents.
The new reports come as international teams continue to trace passengers and monitor symptoms across multiple countries, hoping to contain the outbreak before additional cases emerge.
Health authorities in at least 12 countries are tracking down and monitoring passengers who disembarked the ship on the remote South Atlantic island of St. Helena on April 24, before the deadly outbreak was detected. They are also attempting to trace others who may have come into contact with them.
On Thursday, the World Health Organization (WHO) said eight cases have been reported so far, of which five have been confirmed as hantavirus cases, and the remaining three are suspected.
Three passengers have died in the outbreak—a Dutch couple and a German national—and several others are sick. Symptoms usually develop between one and eight weeks after exposure to the virus.
Investigators in Argentina suspect the Dutch couple may have contracted the virus while on a bird-watching trip before they boarded the cruise ship, The Associated Press reported. The Dutch man died on board the ship, while his wife died after being evacuated to South Africa.
The WHO says the risk to the wider public is low. Hantavirus is usually spread by inhaling contaminated rodent droppings and is not easily transmitted between people.
Countries Trace Dozens Who Disembarked From Cruise Ship
On April 24, more than two dozen people from at least 12 countries disembarked from the ship on St. Helena without contact tracing, the ship’s operator, Oceanwide Expeditions, and Dutch officials said. This was nearly two weeks after the first passenger had died on board.
On April 25, a number of passengers flew from St. Helena to Johannesburg, including the Dutch woman who later died in South Africa. Authorities in South Africa are now trying to trace the contacts of any passengers who got off the ship and traveled to the country.
The passengers include seven from the United Kingdom, six from the United States, three from the Netherlands and two each from Canada, Switzerland, and Turkey. Other passengers who disembarked from the ship on April 24 hail from Germany, Denmark, St. Kitts and Nevis, New Zealand, Singapore and Sweden.
Health authorities first confirmed hantavirus in a ship passenger on May 2. That was a British national admitted to intensive care in Johannesburg, who was in a “critical but stable condition.”
It emerged on Wednesday that a man tested positive for hantavirus in Zurich, Switzerland, after he disembarked at St. Helena, though his precise movements in between are not clear.
Oceanwide Expeditions said the man’s wife “has not shown symptoms but is self-isolating as a precaution.”
A French citizen with “benign symptoms” is in isolation and undergoing medical tests, after being identified as a contact case linked to the flight from St. Helena to Johannesburg, the French Health Ministry said in a statement on Thursday.
Three people, including the ship’s doctor, were evacuated on Wednesday while the ship was near the West African island country of Cape Verde and taken to specialized hospitals in Europe for treatment.
None of the remaining passengers or crew on the ship is currently symptomatic, Oceanwide Expeditions said Thursday. The ship, which has more than 140 passengers and crew members still on board, is now sailing to Spain’s Canary Islands and is expected to arrive at the port of Granadilla on the island of Tenerife on Sunday.
In the U.S., officials in four states—Arizona, California, Georgia, and Virginia—are monitoring residents who have returned home after being on the ship.
New Jersey health officials say two state residents are being monitored after the CDC notified the state of a potential hantavirus exposure involving an infected traveler who had recently departed the MV Hondius cruise ship. According to Gov. Mikie Sherrill, the individuals were not passengers on the vessel; their possible exposure occurred during overseas air travel, not in New Jersey.
Both residents are currently asymptomatic and are being followed in coordination with local health departments. State officials emphasized that there are no confirmed hantavirus cases in New Jersey, and the risk to the public remains very low.
A Dutch flight attendant was also undergoing hantavirus testing after coming into contact in Johannesburg with the Dutch woman who later died from the infection.
The U.K.’s Health Security Agency said two people who returned to the country having been on board the Hondius had been advised to self-isolate but were not reporting symptoms as of Wednesday.
In Singapore, two residents who were on board the ship were being isolated and tested for the virus at the National Center for Infectious Diseases (NCID), CNA reported.
“Their test results are pending. One has a runny nose but is otherwise well, and the other is asymptomatic. The risk to the general public in Singapore is currently low,” NCID said, according to the outlet.
Israel Confirms First Hantavirus Case, Linked to European Strain
Israel has recorded its first hantavirus case in years, after a patient tested positive for a European strain of the virus, according to reporting from Maariv — a strain unrelated to the Andes variant driving the cruise‑ship outbreak. The individual had traveled in Eastern Europe several months earlier and sought medical care after developing symptoms consistent with hantavirus infection.
Health officials say the patient is in stable condition and has not required intensive care or strict isolation. An initial antibody test indicated exposure, and a follow‑up PCR test confirmed the presence of the virus’ genetic material. Authorities have not released identifying details about the patient or the medical facility where the diagnosis was made.
Hantavirus infections are rare in Israel, though several suspected cases were reported about a decade ago among travelers returning from South America. Unlike the Andes strain currently at the center of the international outbreak aboard the Hondius, the strain detected in Israel is not known for person‑to‑person transmission and is typically spread through contact with infected rodents.
Low Transmissibility
“As widely covered, the person-to-person transmissibility of this virus is very low,” Ian Jones, professor of virology at the University of Reading in the U.K. told Newsweek on Thursday. “The main risk is from the original source, rodent droppings and urine, which can become airborne if they are disturbed, for example, by cleaning.”
“Contacts who are very close to the original infected individual, usually family members or nursing staff, can become infected but it does not happen easily and it is not likely that general members of the cruise have been infected,” he said.
Jones added: “Once the incubation period has passed the outbreak will be over and until that time the risk to the general public is effectively nil.”
What Is Hantavirus?
Hantaviruses are a related family of viruses found worldwide, many of which can cause illness in humans. They are generally classified into two groups: “Old World” strains found in Africa, Asia and Europe, and “New World” strains in the Americas. Although related, these groups are associated with distinct diseases—New World hantaviruses cause hantavirus cardiopulmonary syndrome (HCPS), while Old World variants cause hemorrhagic fever with renal syndrome (HFRS).
The Andes virus is the only hantavirus in which infection through human-to-human contact has been documented.
The modern understanding of hantavirus traces back to research in South Korea, where scientists were investigating a mysterious hemorrhagic fever that struck thousands of soldiers during the Korean War. Although the illness had been seen in parts of Eurasia decades earlier, the virus responsible wasn’t isolated until 1978, when Dr. Ho‑Wang Lee identified it in the striped field mouse, a species common near the Hantan River. That discovery led to the naming of the Hantaan virus, the first recognized member of what would become a newly classified viral genus in 1981.
Historical records show the disease had been circulating long before its formal identification. Retrospective analyses uncovered cases in Europe dating back to 1913 and additional evidence from Asia dating to the 1930s, revealing a much longer and broader presence than previously understood.
The virus gained new attention in the United States in 1993, when an unexplained respiratory illness emerged in the Four Corners region. Investigators eventually identified a previously unknown strain—later named the Sin Nombre virus—which caused Hantavirus Pulmonary Syndrome, a severe and often fatal disease distinct from the hemorrhagic fever seen in Asia.
What is the Andes strain?
The Andes strain is one of the most severe hantaviruses known to science, part of a family of rodent‑borne pathogens that have likely existed for as long as their hosts. While hantaviruses are found worldwide, the Andes virus stands out as the only strain in the Americas known to spread from person to person, a feature that sets it apart from other New World and Old World variants.
The Andes virus belongs to the New World hantaviruses, which tend to cause hantavirus pulmonary syndrome, a rapidly progressive respiratory illness with a high fatality rate. These American strains are generally more dangerous than the Old World hantaviruses found in Europe and Asia, which more often cause kidney‑related disease.
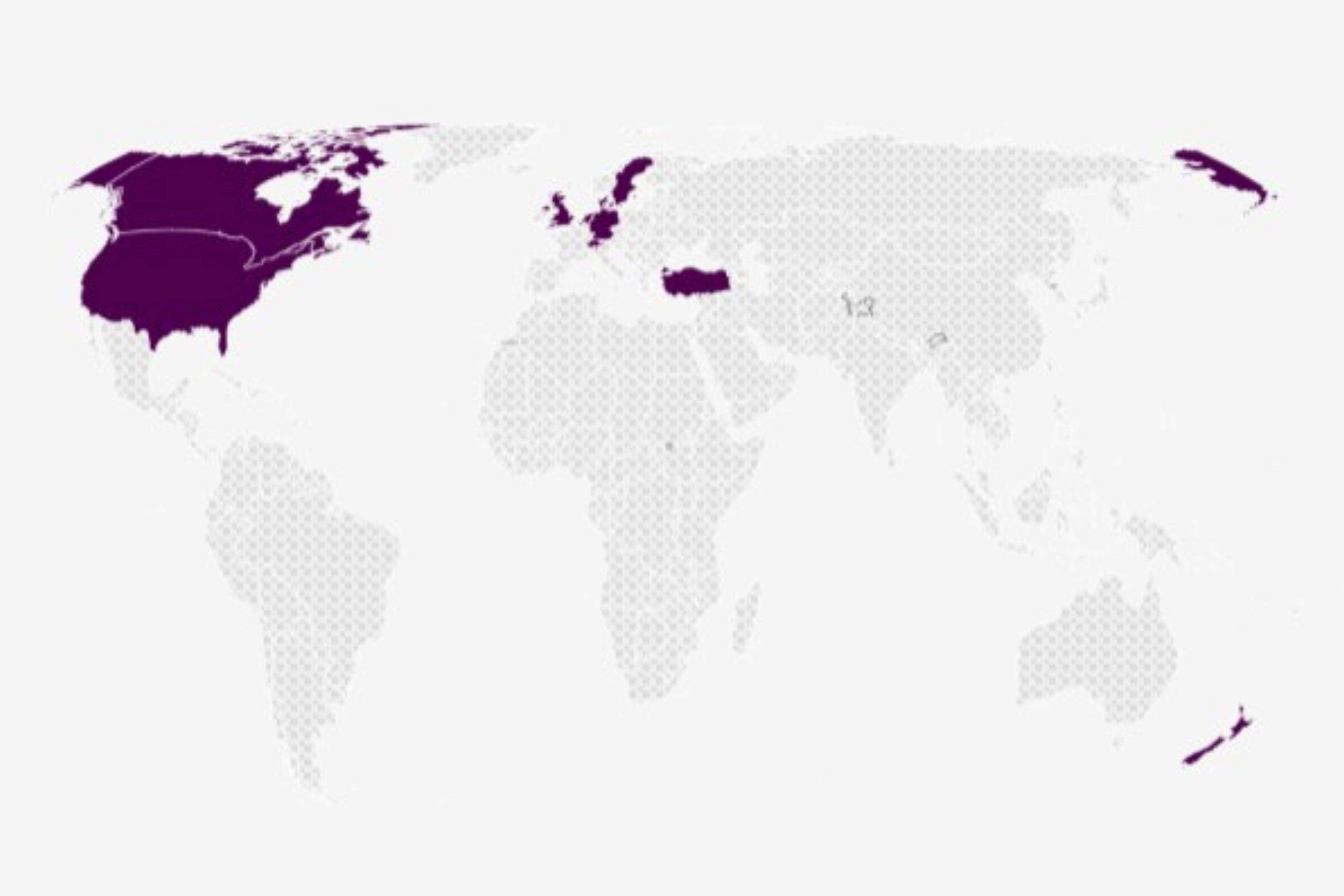
List of Locations Where Latest Hantavirus Strain is Being Monitored
How Hantavirus Compares to Covid-19
Hantaviruses are spread through rodent droppings and urine, particularly when dried particles become airborne during cleaning. Sweeping out an old storeroom, as the worker had done, is a classic scenario for exposure. In the United States, fewer than 1,000 cases have been reported since tracking began in 1993, most of them in rural areas of the West.
The illness typically starts with fever, fatigue, muscle aches, and headache, then progresses over several days to coughing, rapid heartbeat, and severe breathing trouble. Some people also develop gastrointestinal symptoms. Because these early signs overlap with those of COVID‑19 and other viral infections, doctors rely on a combination of specialized blood tests and a patient’s exposure history to confirm hantavirus infection.
HPS is considered a medical emergency, with a fatality rate of nearly 40%. Treatment focuses on supporting the lungs and heart as the body fights the infection, often requiring oxygen therapy or mechanical ventilation.
There is no vaccine for hantavirus, but the virus is easily destroyed by disinfectants. Experts recommend wearing gloves, long sleeves and an N95 mask when cleaning areas where rodents may be present. In heavy infestations, professional pest control is the safest option. Anyone who develops flu‑like symptoms after rodent exposure should seek medical care promptly and mention the potential contact.
Related Articles